Early development
Telepathology, the remote practice of pathology, originates from a need for quick remote consultation. In an increasingly technologically connected world, communication and collaboration have become more convenient, particularly benefiting healthcare practices. In the decades since its development, telepathology has grown more useful than ever before, allowing pathologists to enhance their practices worldwide with faster and more accurate results.

Remote pathology was introduced in the 1980s. Data gathered at the end of a clinical trial by the National Bladder Cancer Project (NBCP) from multiple institutions across the U.S. determined large discrepancies in the diagnoses given. Dr. Ronald S. Weinstein, Director of the Central Pathology Laboratory (CPL) for the NBCP, was encouraged to develop a system for CPL uropathologists to analyze patient data from these contributing institutions.
However, the time between surgery and entry into clinical trials was very short and technology at the time could not support immediate remote pathology, hence dynamic-robotic telepathology was developed. Dynamic-robotic microscopy was first brought to market in 1985. In its most simple form, it is a satellite-controlled microscope that allows for remote analysis of slides. This was the first tool to enable remote pathology and initiated a technological progression still being cultivated today.
Dr. Weinstein devised the term “telepathology” to encompass the field this new technology would support and publicized it during a lecture at the Armed Forces Institute of Pathology (AFIP) in 1986. The same year, the first public demonstration of the robotic microscope was held. A pathologist in Washington D.C. analyzed and diagnosed a breast biopsy through remote control of a microscope located nearly 2,000 miles away in El Paso, Texas. The event was a great success and an optimistic beginning to a new field of medicine.
Technological expansion
In the early 1990s the first telepathology network was established in Norway. The University Hospital in Tromsø began providing frozen section services to five remote hospitals in the north of the country. Pathologists in Tromsø could analyze frozen tissue samples in real time from transmitted video images, while located hundreds of kilometers from the patient. This was especially valuable for hospitals with a lack of specialists and supported the rapid nature of intraoperative diagnosis.
Over the last few decades telepathology has developed significantly in parallel with new technology, such as whole slide imaging (WSI) that came to market in 2000. These digital scans of slides are easily stored, duplicated, and shared worldwide. Since its inception WSI has become widely used. Today’s commercially available WSI scanners from companies like Leica and Hamamatsu to name a few, are capable of automatically creating high-resolution images rapidly from glass slides.
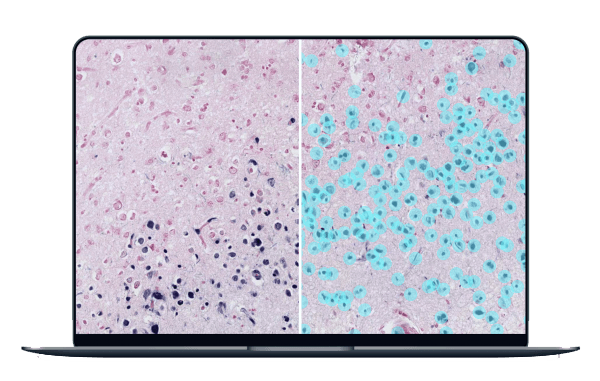
WSI and the digitization of these images has in turn promoted the use of Artificial Intelligence (AI) in image analysis, which enables faster and more accurate data processing. AI-assisted analysis and even diagnosis also decreases cognitive and visual inter- and intra-observer biases. Easier diagnosis subsequently accelerates therapy, avoiding further development of a patient’s illness.
Telepathology today
During the COVID-19 pandemic, telepathology surged due to limited in-person work and a need for worldwide collaboration. In March of 2020 the Centers for Medicare & Medicaid Services (CMS) in the United States allowed pathologists to temporarily work from home. While there are only two approved digital pathology devices, an FDA policy from April allows provisional use of devices beyond those officially approved, including scanners, viewing software, and remote recording devices.
As people accustom to remote work, technological progress in telepathology is ever more important and the benefits far reaching, such as:
- Remote work: telepathology accommodates remote work, particularly during the pandemic, perhaps even shifting the paradigm for pathology in the future. Healthcare access to remote places is also easier with less need for patients or doctors to travel.
- Speed and accuracy: The development of AI technology delegates image analysis work to computers, leading to faster and more accurate results. This also increases healthcare quality through standardizing care and shortening the delay between diagnosis and therapy.
- Collaboration: Ability to ask for second opinions on complicated cases from colleagues and refer patients to specialists worldwide without the need to send physical slides or meet in person is also a huge advantage.
Explore Aiforia’s cloud-based solutions for pathology.
References
Aeffner, Famke et al. Introduction to digital image analysis in whole-slide imaging: A white paper from the digital pathology association https://doi.org/10.4103/jpi.jpi_82_18
Aiforia Telepathology Webinar: https://info.aiforia.com/telepathology-webinar
Julien Meyer, Guy Paré. Telepathology Impacts and Implementation Challenges: A Scoping Review https://doi.org/10.5858/arpa.2014-0606-RA
Krupinski E.A., Bhattacharyya A.K., Weinstein R.S. Telepathology and Digital Pathology Research. https://doi.org/10.1007/978-3-319-20379-9_5
Magdala de Araújo Novaes. Chapter 10 - Telecare within different specialties. https://doi.org/10.1016/B978-0-12-814309-4.00010-0